CLINICAL SERVICES

Telehealth For Patients At Home

Our Remote Care Teams monitor patients daily.
We help to coordinate care across providers.
Remote Physiological Monitoring (RPM)
Remote Physiological Monitoring (RPM) simply monitors patients remotely! RPM requires an FDA-cleared device capable of collecting physiological data (BP, BG, SpO2, weight, and temperature) in one location and electronically transmitting those data to the remote care team at a different location. OTAi staff monitor the incoming readings daily, we call patients by phone monthly, and communicate with patients, family, caregivers, and physician-led care teams throughout the month by text, email and EMR.

Chronic Care Management (CCM)
Chronic Care Management (CCM) brings structure to patient care delivered remotely – between office visits. Designed for patients “with two or more chronic conditions expected to last at least 12 months or until the patient’s death, and place the patient at significant risk of death, acute exacerbation, or functional decline.” Medicare introduced CCM more than ten years ago to incentivize healthcare providers to maintain monthly contact with patients by phone, email, and text. This high-touch, remote care model has proven effective at early detection, early intervention, reduced visits to the ER, reduced hospital admissions, and generally improved patient outcomes.

The Physician’s Care Plan guides and informs engagement during our monthly patient check-in calls.
Prinicpal Care Management (PCM)
Principal Care Management (PCM) is a set of non face‑to‑face care management services for patients who have a single serious or high‑risk chronic condition that is expected to last at least 3 months and requires focused, ongoing management and coordination by one clinician. It is similar to Chronic Care Management but is centered on monitoring one (principal) condition, rather than multiple conditions

Remote Therapeutic Monitoring (RTM)
Remote Therapeutic Monitoring (RTM) collects non-physiological patient data to monitor a patient’s care plan adherence, symptoms, mood, medication adherence, mental cognition, memory loss, physical mobility, and general response to therapy. RTM is increasingly being used to monitor patient’s response to therapy, for patients with depression, anxiety, and a range of other mental and behavioral conditions. RTM also enables patient-reported data collection and analysis.

Care Plans And Clinical Workflows
A collaborative, protocol-driven approach maximizes the utility of telehealth in Ophthalmology. We monitor chronic eye disease via a daily review of physiological and non-physiological data. Our remote care teams also host monthly patient checkin calls. During our patient “check-in” calls we share information, review symptoms, monitor adherence to medication and care plan guidance, assess patient’s response to therapy, and prompt an escalation alert – when indicated. This helps to drive patient compliance and improve outcomes.
TURNKEY SOLUTIONS

Turnkey Solutions for RPM, CCM, PCM, and RTM deliver a streamlined and effective path for healthcare providers to deliver high-quality, compliant telehealth services while maximizing operational efficiency and revenue.
Benefits of Turnkey Telehealth Solutions
- Rapid Implementation: Providers can launch new programs without building internal infrastructure.
- Scalability: Easily expand to more patients or services as demand grows.
- Regulatory Compliance: Solutions are designed to meet HIPAA and CMS requirements, reducing risk.
- Operational Efficiency: Outsourcing logistics and support allows clinical staff to focus on patient care.
- Improved Outcomes: Enhanced patient engagement and proactive monitoring lead to better health results.
Turnkey RPM services provide end-to-end support for remotely tracking patient health data for chronic disease management. Key features include:
- Device Provisioning and Setup: Sourcing, delivering, and configuring monitoring devices for patients.
- Patient Onboarding and Support: Handling consent, education, and troubleshooting to ensure patients can use devices effectively.
- Data Collection and Integration: Securely capturing real-time patient health metrics and integrating with EHRs or provider dashboards.
- Clinical Monitoring: Optional services where clinical teams review data, respond to alerts, and communicate with patients as needed.
- Compliance and Billing: Ensuring all processes meet HIPAA and CMS requirements, with support for accurate and timely reimbursement.
- Operational Efficiency: Providers can focus on clinical care while we manage logistics, tech support, and patient engagement, reducing staff burden and improving outcomes.
Turnkey CCM services automate and streamline the management of patients with multiple chronic conditions. Key components include:
- Care Plan Creation and Documentation: Tools for building condition-specific care plans, tracking interventions, and updating progress notes.
- Automated Time Tracking: Capturing time spent on care coordination to ensure compliance with CMS billing requirements.
- Role-Based Access: Secure, HIPAA-compliant platforms with customizable access for different care team members.
- Reporting and Analytics: Dashboards for monitoring program performance, patient engagement, and reimbursement metrics.
- Integration with RPM: Many turnkey CCM solutions are designed to work seamlessly with RPM, enabling holistic, value-based care.
Turnkey RTM services monitor patient adherence to therapy regimens for musculoskeletal or respiratory conditions. Core features include:
- Automated Patient Engagement: Regular check-ins, motivational interviews, and coaching to maximize adherence.
- Home Exercise Programs: Platforms may include digital exercise libraries and compliance tracking.
- Time and Communication Tracking: Automatic logging of required two-way audio interactions and other billable activities.
- Billing and Revenue Cycle Management: Ready-to-submit CPT codes and revenue-sharing models to simplify reimbursement.
- Compliance Monitoring: Ensuring all interactions and data collection meet CMS and payer requirements.
PLATFORM LICENSING
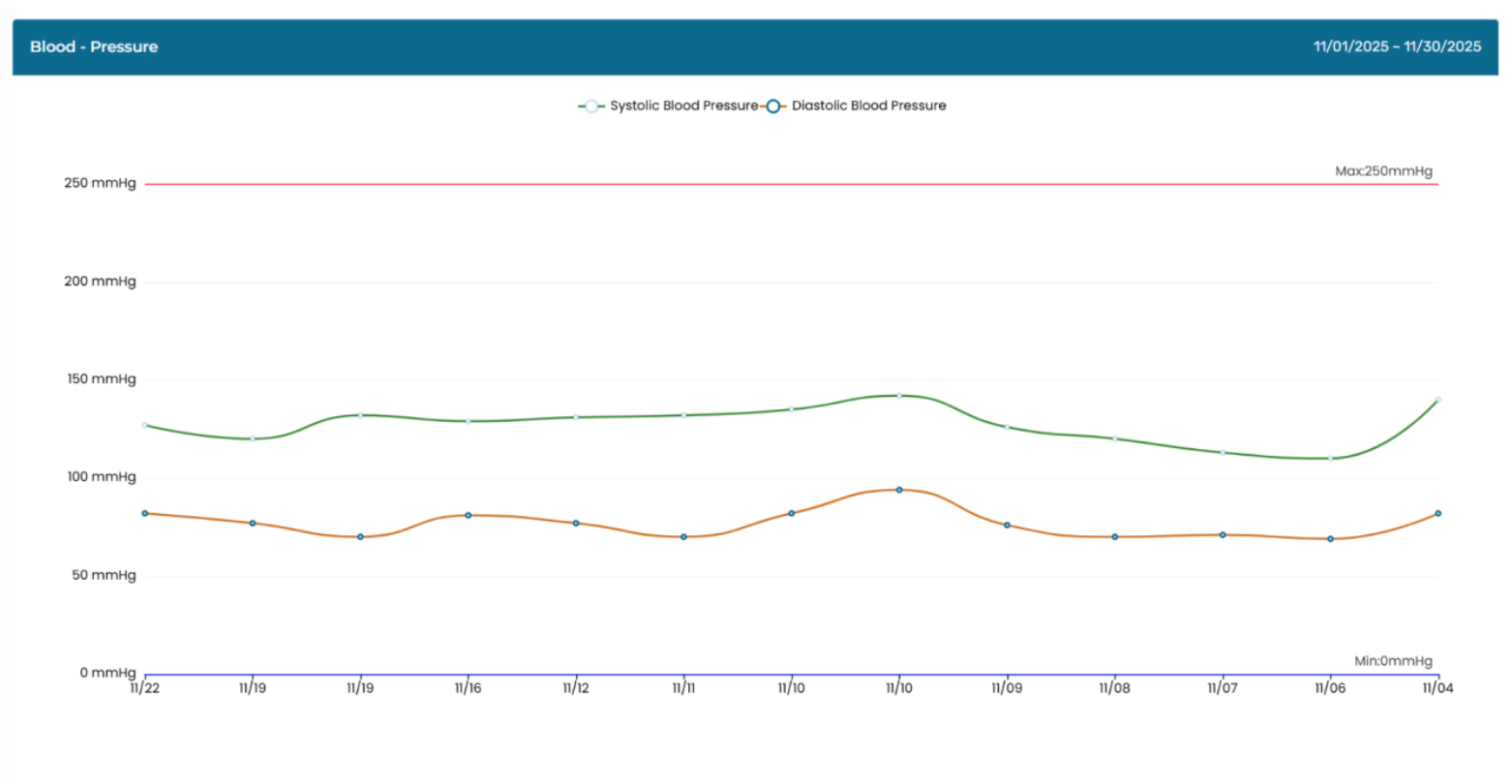
Licensing our telehealth platform offers hospitals and clinics a range of strategic, clinical, and operational benefits. These advantages improve patient care, optimize resources, and position healthcare organizations for future growth. Contact us to schedule a demo.
Expanded Access to Care breaks down geographic barriers, enabling hospitals to reach patients in rural or underserved areas and connect them with specialists who may not be available locally. It extends the hospital’s services beyond its physical location, increasing its catchment area and patient base.
Operational Efficiency and Cost Savings Virtual care reduces the need for in-person visits, which can lower overhead costs associated with clinic space, staffing, and patient throughput. We can help decrease hospital readmissions and emergency department overcrowding by enabling remote follow-ups and triage. Shared staffing models and remote consultations allow hospitals to optimize specialist resources and reduce duplication of services.
Enhanced Patient Experience and Engagement offers patients greater convenience and flexibility, allowing them to attend appointments from home and fit healthcare into their schedules more easily. Features like secure messaging, appointment reminders, and access to medical records empower patients to take an active role in their care, leading to higher satisfaction and better outcomes. Improved Continuity and
Quality of Care Regular virtual check-ins support chronic disease management, medication adherence, and ongoing monitoring, ensuring consistent care even outside the hospital setting. Remote monitoring tools and wearable devices enable real-time tracking of patient health, allowing for timely interventions and personalized care plans.
Infection Control and Safety By reducing the number of in-person visits helps limit the spread of infectious diseases, protecting both patients and staff.
Streamlined Clinical Workflows include features for clinician-to-clinician communication, which streamline processes and reduce administrative burdens. Hospitals can better coordinate care, share information securely, and manage patient flow more efficiently.
Scalability positions hospitals to adapt to evolving patient expectations and healthcare delivery models, including hybrid care (combining in-person and virtual services). Technology enables hospitals to quickly scale services up or down in response to public health emergencies or changing demand.
REMOTE CLINICAL STAFFING

Outsourcing Staff to operate your telemedicine platform offers several strategic and operational advantages for healthcare providers. These benefits span cost savings, scalability, efficiency, and improved patient care.
Cost Savings and Financial Flexibility made possible by eliminating the need to hire, train, and house additional in-house staff, reducing overhead costs such as salaries, benefits, office space, and equipment. Providers can save up to 70% on staffing expenses by leveraging outsourced medical assistants. The contractual nature of outsourced staffing allows organizations to pay only for the services they need, freeing up resources for investment in other critical areas like technology or clinical training.
Scalability and Flexibility through outsourced staffing models allow healthcare providers to scale their workforce up or down quickly in response to fluctuating patient volumes, seasonal demand, or expansion into new service areas. This flexibility is especially valuable during emergencies, busy seasons, or when expanding telemedicine services to new regions or time zones.
Access to Expertise and Expanded Talent Pool connects healthcare providers with certified medical assistants who are experienced in telemedicine, familiar with the latest technologies, and trained in compliance with medical guidelines and data privacy regulations (e.g., HIPAA). Providers can tap into a broader pool of talent, including individuals with specialized knowledge, language abilities, and telemedicine-specific skills, regardless of geographic location.
Operational Efficiency and Reduced Administrative Burden by shifting essential administrative tasks such as appointment scheduling, patient onboarding, reminders, follow-ups, and billing, streamlining telemedicine workflows and reducing the risk of errors or missed appointments. By delegating these time-consuming tasks, healthcare providers can focus more on direct patient care, improving both provider satisfaction and patient outcomes.
Enhanced Patient Experience and Engagement enabled by improved communication by sending timely reminders, guiding patients through onboarding, and ensuring follow-ups are handled efficiently, which reduces no-show rates and enhances patient satisfaction. Their support helps patients navigate telemedicine platforms, fosters trust, and encourages active participation in their care, which is particularly valuable for chronic disease management and ongoing remote monitoring.
Remote Patient Monitoring (RPM)
Remote patient monitoring (RPM) is a healthcare delivery method that uses digital technology to monitor patients outside traditional clinical settings, such as at home. RPM involves the use of connected medical devices-like blood pressure monitors, blood glucose meters, pulse oximeters, weight scales, and wearable sensors-to collect a wide range of physiological and health data from patients. This data is then electronically transmitted to healthcare providers for ongoing assessment and management.
2025 Remote Patient Monitoring (CPT) Codes
| 99453 | Initial set-up & patient education on equipment (one-time fee). | $22.25 |
| 99454 | Supply of devices, Data collection and transmission, 16 days per month. | $49.04 |
| 99457 | Remote physiologic monitoring services by clinical staff/MD/ QHCP first 20 cumulative minutes of RPM services over a 30-day period. | $52.23 |
| 99458 | Remote physiologic monitoring services by clinical staff/MD/ QHCP for an additional cumulative 20 minutes of RPM services over a 30-day period. | $42.42 |
| 99091 | Collection and interpretation of data by physician or QHCP, 30 minutes. | $54.22 |
Chronic Care Management (CCM)
Chronic Care Management (CCM) is a structured healthcare service designed to support individuals with two or more chronic health conditions that are expected to last at least 12 months or until the patient’s death, or that place the patient at significant risk of death, acute exacerbation, or functional decline. CCM is covered by Medicare and most private insurance providers.
2025 Chronic Care Management (CPT) Codes
| 99490 | Minimum 20 cumulative minutes over a 30-day period of non-face-to-face time monitoring the care plan. | $66.94 |
| 99439 | Subsequent 20 minutes of care provided by clinical staff. | $50.37 |
| 99491 | Initial 30 minutes of care personally provided by physician, or non-physician practitioner (NPP). | $91.45 |
| 99437 | Subsequent 30 minutes of care personally provided by a physician or NPP. | $64.36 |
Remote Therapeutic Monitoring (RTM)
Remote Therapeutic Management (RTM) is a healthcare service that uses digital technology to remotely monitor and manage a patient’s therapy, particularly for chronic conditions affecting the musculoskeletal or respiratory systems. The primary focus of RTM is on collecting and assessing non-physiological patient data-such as symptoms, therapy adherence, medication response, and self-reported outcomes-rather than physiological metrics like blood pressure or glucose levels.
2025 Remote Therapeutic Monitoring (RTM) Codes
| 98975 | Remote therapeutic monitoring (e.g., respiratory system status, musculoskeletal system status, therapy adherence, therapy response); initial set-up and patient education on use of equipment | $22.25 |
| 98976 | RTM (respiratory); supply 16 readings per month. See “98977” | $49.04 |
| 98977 | RTM (musculoskeletal); device(s) supply with scheduled (e.g., daily) recording(s), manual reporting by patient, and/or programmed alert(s) transmission to monitor musculoskeletal system, each 30 days [16 readings minimum each 30 days] | $49.04 |
| 98980 | At least 20 minutes of clinical staff time directed by a physician or other qualified health care professional, per calendar month, requiring at least one interactive communication with the patient/caregiver during the calendar month | $52.23 |
| 98981 | Each additional 20 minutes of clinical staff time directed by a physician or other qualified health care professional, per calendar month (list separately in addition to code for primary procedure) | $42.42 |








